UDK: 616-089.844-089.5-056.257
Peev I.
1University Clinic for Plastic and Reconstructive Surgery Faculty of Medicine, Ss. Cyril and
Methodius University, Skopje, Republic of North Macedonia
Abstract
Tumescent local anesthesia has revolutionized the field of liposuction and body contouring by enabling large-volume fat removal with minimal blood loss and enhanced patient safety. This technique involves the subcutaneous infiltration of a dilute solution of local anesthetic (commonly lidocaine) and epinephrine, producing profound regional anesthesia, vasoconstriction, and tumescence of the targeted tissue. When combined with analgosedation, particularly with short-acting agents such as remifentanil and dexmedetomidine, it offers a balanced approach between patient comfort and procedural control.
Remifentanil, an ultra–short-acting opioid, provides potent analgesia with rapid onset and offset, allowing precise titration to surgical needs and a smooth recovery profile. Dexmedetomidine, a selective α2-adrenergic agonist, provides anxiolysis, sedation, and analgesic-sparing effects while maintaining respiratory stability-a key advantage in procedures performed under local anesthesia. The synergistic combination of these agents minimizes intraoperative discomfort, reduces the need for higher doses of lidocaine, and improves overall patient tolerance. This review summarizes current evidence and clinical experience supporting the use of tumescent local anesthesia with remifentanil–dexmedetomidine sedation in liposuction and liposculpture. The approach enhances patient satisfaction, optimizes perioperative hemodynamics, and ensures faster recovery with a low incidence of complications, making it an increasingly preferred modality in modern aesthetic surgery.
Keywords: analgosedation, dexmedetomidine, remifentanil, liposuction ,tumescent local anesthesia.
Introduction
The number of body contouring procedures has increased globally and liposuction has become the second most common cosmetic procedure. This aesthetic surgical procedure removes excess fat from a specific region of the body, most commonly from the abdomen, hips, thighs, upper arms and additional body areas (1). The combination of removing fat from one body region and reusing it in terms of lipofilling or fat grafting in others is called liposculpture. Liposculpture aims to model and define the contours of the body to achieve a more aesthetic, natural, and harmonious appearance (2).
With the rising demand for body contouring procedures, many hospitals are transitioning these procedures to one-day (ambulatory) surgical settings, aiming to reduce healthcare costs and decrease the incidence of postoperative complications for patients (1). It is prudent for the anesthesiologist to be familiar with the techniques used to facilitate liposuction, the options for anesthesia, and the recognition and management of complications in order to provide safe care to patients (3,4).
Modern era of liposuction began in the 1970s./80s with the work of Giorgio Fischer, who introduced the “dry technique” using a cannula, a method with considerable postoperative morbidity and blood loss of up to 25 % of the aspirated volume. A pivotal peer advancement occurred in France, where Yves-Gerard Illouz and Pierre Fournier refined the so-called “wet technique”, incorporating vacuum cannulas and wetting tissue solutions, an approach that significantly improved effectiveness of fat removal procedures and moreover, the safety of the patients (5,6). In 1987, Jeffrey A. Klein introduced the concept of tumescent local anesthesia (TLA), a development that fundamentally transformed the practice of liposuction. The tumescent technique, which involves infiltration of large volumes of dilute local anesthetic and vasoconstrictor solution, greatly enhanced patient comfort, minimized bleeding, and became the gold standard of care in contemporary liposuction practice that can even be performed ambulatory (7-10). Modern advancements in technology and technique have further expanded the scope and precision of body contour. And lately, high-definition liposculpture (HD liposculpture) has been developed to accentuate and define muscular contours, particularly in areas such as the abdomen, flanks, and torso (11).
Contemporary methods incorporate energy-assisted modalities, such as ultrasonic-assisted liposuction, which selectively targets fat cells while preserving connective tissue, as well as PAL (Power Assisted Liposuction), which enhances fat removal efficiency and surgeon control (12,13).
Tumescent Local Anesthesia (TLA) Technique
The tumescent technique is the most commonly used method of local anesthesia in liposuction. It involves subcutaneous infiltration of large volumes of fluids containing highly diluted local anesthetic (usually lidocaine) combined with epinephrine, resulting in tissue oedema and firmness that facilitates both anesthesia and hemostasis. Originally developed for liposuction, its use has expanded to other surgical procedures, including plastic surgery, breast, ENT, and vascular surgery (14,15). TLA provides effective local anesthesia, often eliminating the need for general anesthesia in massive liposuction, significantly reduces blood loss and bruising through epinephrine-induced vasoconstriction and hydrostatic compression, decreases postoperative pain and extends analgesia due to slow systemic absorption of lidocaine, and furthermore, it facilitates quicker recovery with lower complication rates compared with procedures under general anesthesia (16-18). Liposuction can be classified by aspirate volume into small-volume (<4 L) and large-volume (>4 L) procedures. Larger volumes of tumescent solution are required for high-volume liposuction, underscoring the importance of careful fluid management and monitoring to mitigate fluid-related complications (19.20).
Tumescent / Wetting Solutions
The classic formulation described by Klein includes lidocaine diluted in 0.9% isotonic saline (approximately 0.05–0.10% lidocaine concentration), epinephrine at 1: 1,000,000 concentration, and sodium bicarbonate to buffer the acidity and facilitate analgesia (21,22). While isotonic saline as a diluent is associated with a burning sensation upon infiltration, lactated Ringer’s solution is not, and it reduces the sodium load (23). Therefore, there are modifications of the original solution, like the one according to Hunstadt (19). [Table 1].
Table 1. Types of wetting solution
| Klein’s solution | Hunstadt’s solution |
| 1000 ml Normal saline | 1000 ml Ringer’s lactate |
| 50 ml, 1% lignocaine | 50 ml, 1% lignocaine |
| 1 ml, 1:1,000 epinephrine
12.5 ml, 8.4% sodium bicarbonate |
1 ml, 1:1,000 epinephrine |
Local Anesthetics
Lidocaine is the most commonly used local anesthetic in tumescent liposuction solutions. In standard local infiltration with epinephrine, the maximum recommended dose is 7 mg/kg; however, the pharmacokinetic properties of tumescent anesthesia allow much higher total doses because of delayed systemic absorption and reduced peak plasma levels. For liposuction, the recommended maximum lidocaine doses are generally 35–45 mg/kg, with accepted safe limits up to 55 mg/kg in most patients when epinephrine is included in the solution. Peak plasma lidocaine levels typically occur several hours after infiltration and remain below toxic thresholds due to slow absorption and removal of some anesthetic during fat aspiration. Factors that further reduce systemic uptake and toxicity risk include low blood flow in subcutaneous fat, vasoconstriction from epinephrine, and sequestration of lidocaine in adipose tissue. Lidocaine is predominantly metabolized in the liver by CYP3A4 and CYP1A2; therefore, doses should be reduced in patients who take drugs that inhibit these enzymes or in patients with impaired hepatic function, as this may increase the risk of systemic toxicity (24-26).\
Vasoconstrictors, Sodium Bicarbonate, and Steroids
Vasoconstrictors decrease tissue blood flow and delay the systemic absorption of local anesthetics, enhancing the safety of tumescent anesthesia. Epinephrine is the most widely used vasoconstrictor in tumescent solutions, with recommended concentrations of 0.25–1 mg/L, adjusted according to tissue vascularity (higher in more vascular areas and lower in less vascular regions). The total epinephrine dose should not exceed 50 μg/kg, and if this limit is likely to be exceeded, the procedure may be staged to reduce the risk. In an alternative approach, Lalinde et al. used l-ornithine 8-vasopressin at 0.01 IU/mL in chilled saline, reporting reduced blood loss compared with conventional epinephrine-containing solutions (27-30).
Sodium bicarbonate is added to tumescent anesthetic solutions to raise the pH and reduce acidity, which significantly reduces the pain and the burning sensation associated with injection of acidic lidocaine-epinephrine mixtures. This buffering increases the proportion of non-ionized lidocaine, facilitating faster diffusion into nerve fibers and improving patient comfort. (29-33). Steroids, especially triamcinolone acetat, as anti-inflammatory additive have been shown to exert anti-inflammatory and circulatory stabilizing effects when added to tumescent solutions, potentially reducing tissue inflammation and postoperative swelling (34).
Preoperative Assessment
Comprehensive preoperative evaluation and optimization of comorbid conditions are essential. Severe cardiovascular disease, active coagulation disorders, and pregnancy are contraindications for liposuction. A detailed history, including all medications, herbal products, and supplements, should be obtained while anticoagulants or drugs that may interfere with lidocaine metabolism (e.g., CYP3A4 inhibitors) should be discontinued. Preoperative investigations typically include complete blood count with platelet assessment, coagulation profile (prothrombin time (PT), activated partial thromboplastin time (aPTT)), liver function tests, and pregnancy testing in women of childbearing age. Perioperative pharmacological and mechanical thromboprophylaxis (e.g., low-molecular-weight heparin and sequential compression devices) should be considered in high-risk patients to reduce the risk of venous thromboembolism. Additional tests—such as ECG, renal function, or specialized cardiac evaluation—may be indicated based on patient age, clinical history, or ASA classification. Preoperative anxiolysis may be provided to reduce procedural anxiety and attenuate related hemodynamic responses (e.g., tachycardia, hypertension, arrhythmias). Oral alprazolam (0.25–0.5 mg) the night before and on the morning of surgery is commonly prescribed for this purpose (31,33,35,36).
Anesthesia Technique
Liposuction can be performed under local, regional (neuraxial), or general anesthesia, alone or in combination. No single technique has been definitively shown to be superior; the choice of anesthesia depends on the patient’s clinical profile, areas treated, and planned volume of aspirate, as well as considerations for day-case versus inpatient surgery (35-37).
Local techniques such as tumescent local anesthesia (TLA) or monitored anesthesia care with sedation are commonly used for small volume or localized liposuction, allowing ambulatory procedures with faster recovery and reduced anesthetic risk. In contrast, general anesthesia is typically preferred for large volume liposuction or when more extensive surgical areas are treated, as it provides complete analgesia, immobility, and facilitated airway control (37). Large volume procedures are associated with risks of late-onset local anesthetic systemic toxicity (LAST) and significant hemodynamic shifts, often necessitating inpatient monitoring (28).
The combination of TLA with analgosedation offers the benefits of limited bleeding and intrinsic analgesia, allowing consideration of ambulatory procedures with earlier recovery and lower costs. Paradigm shift is successfully used in larger liposuctions with/without fat grafting, especially when the patient’s cooperation is needed (patient’s position has to be changed) (28,29). It substitutes general anesthesia, thus shortening the operating time when patient mobility is acquired. However, intensive intraoperative monitoring by the anesthesiologist and accurate titration of sedation are required continuously. Commonly used sedative agents for TLA include midazolam, propofol, ketamine, clonidine, or dexmedetomidine, with supplemental opioids such as fentanyl or remifentanil as required; however, the primary analgesia facilitating the procedure is provided by the TLA itself (25-27).
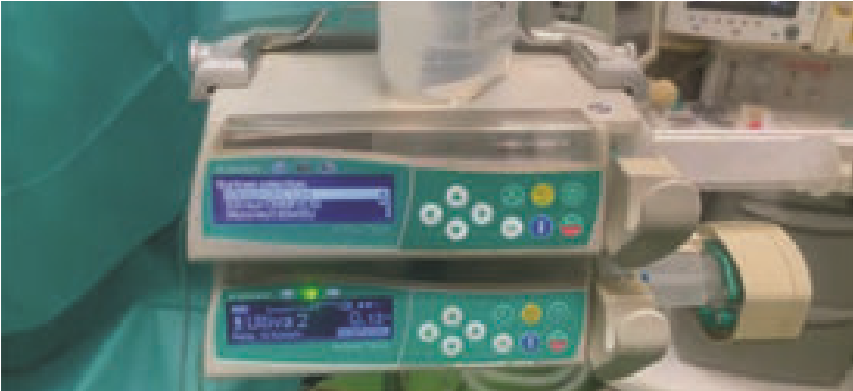
Sedation and analgesia for liposuction can be effectively achieved with dexmedetomidine combined with adjuncts such as remifentanil. (Fig 1). This combination provides reliable sedation and analgesia while maintaining hemodynamic stability and satisfactory operative conditions. A common challenge with dexmedetomidine–remifentanil sedation is balancing adequate depth of sedation with preservation of spontaneous respiration. Dexmedetomidine produces sedative and hypnotic effects via α₂-adrenergic receptors in the locus coeruleus, offering sedation with relatively minimal respiratory depression, whereas remifentanil—being a ultra-short-acting opioid—carries a higher risk of respiratory depression (29,30). Esketamine, the S-enantiomer of ketamine, may counteract opioid-induced respiratory depression and enhance analgesia when used as an adjunct. Perioperative low-dose esketamine has been associated with improved postoperative comfort, reduced anxiety, better sleep quality, and enhanced patient and surgical team satisfaction when combined with dexmedetomidine and remifentanil in liposuction anesthesia. These effects are likely attributed to its N-methyl-D-aspartate receptor (NMDAR) antagonism and sympathomimetic properties that support hemodynamic stability (31-34).
Figure 1. Perfusor with dexmedetomidine and remifentanil
Monitoring
Standard anesthesia monitoring is mandatory for all patients undergoing liposuction, regardless of the anesthetic technique used. This should include continuous assessment of pulse oximetry (SpO₂), non-invasive blood pressure (NIBP), electrocardiogram (ECG), end-tidal carbon dioxide monitoring (capnography) when sedation is administered, and temperature, to enable early detection of physiological changes and maintenance of homeostasis (35).
For patients under sedation, continuous capnography is essential to assess ventilation and detect hypoventilation or airway obstruction early, in line with recognized anesthesia monitoring standards. Routine non-invasive monitoring may suffice for small-volume procedures. Highrisk patients or those undergoing large-volume liposuction often require enhanced monitoring, such as invasive arterial blood pressure measurement and central venous pressure monitoring, due to the potential for significant fluid shifts and hemodynamic alterations (36). In lengthy procedures, insertion of a urinary catheter is useful for monitoring hourly urine output as a surrogate for intravascular volume status and overall fluid balance. Regular urine output assessment helps guide fluid therapy and detect early signs of hypovolemia or fluid overload (34-36).
Patient Positioning
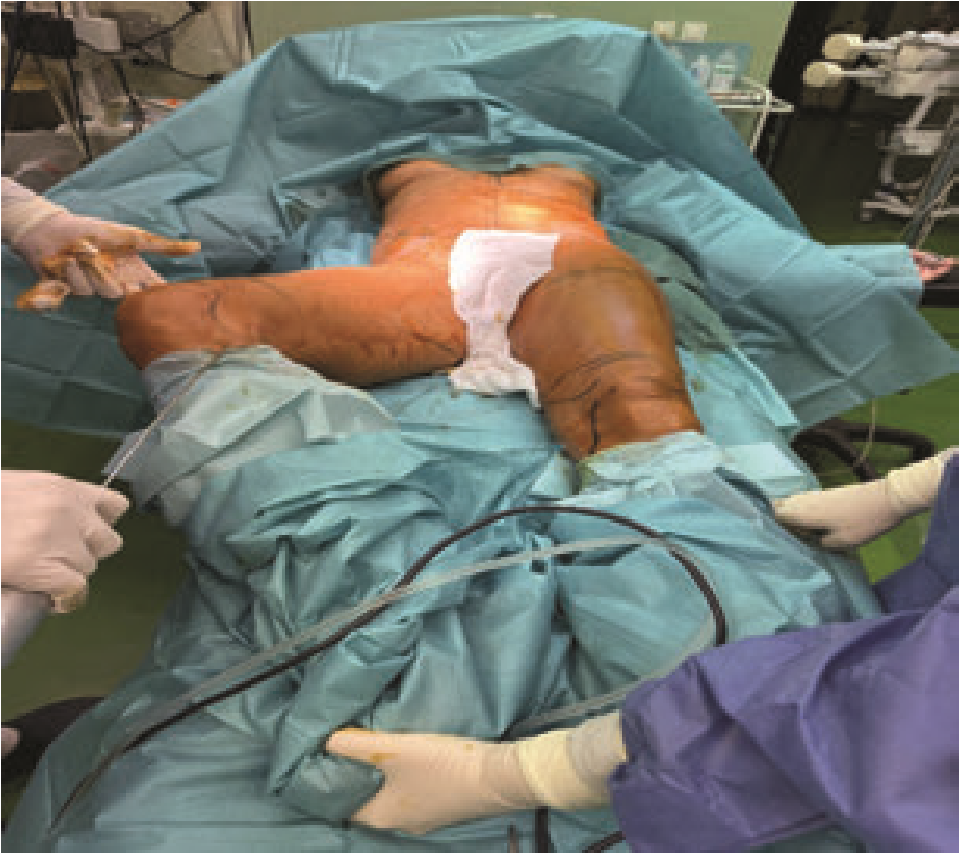
Patient positioning during liposuction is determined by the anatomical area being treated; while the supine position is most common, areas such as the buttocks and posterior thighs may require prone positioning to allow optimal surgical access. Careful attention must be paid to padding pressure points to prevent nerve and soft-tissue injuries—this includes cushioning the face, breasts, iliac crests, knees in the prone position, and the elbows and heels in the supine position. Protection of the eyes, for example with lubrication and padding, is essential when patients are prone to avoid corneal injury. (Figure 2) For large-volume liposuction and prolonged procedures, the use of intermittent pneumatic compression devices on the lower limbs is recommended intraoperatively to reduce the risk of deep vein thrombosis (DVT) and support thromboembolism prophylaxis (37).
Figure 2. Infiltration of TLA
Hemodynamics
While small-volume liposuction is generally well tolerated with minimal hemodynamic disturbance, large-volume liposuction (defined as > 4 L of aspirate) is associated with significant cardiovascular changes during the perioperative period (25). Studies of large-volume liposuction demonstrate increases in cardiac index, heart rate, mean pulmonary arterial pressure, stroke volume index, and right ventricular work index, often accompanied by decreases in mean arterial pressure and systemic vascular resistance. These changes reflect a state of relative hyperdynamic circulation and fluid redistribution during the procedure (26,27). The routine use of large doses of epinephrine to achieve vasoconstriction and a relatively bloodless field can contribute to tachycardia and elevated cardiac output, as higher circulating catecholamine levels augment cardiac performance. In contrast, the observed reduction in systemic vascular resistance and mean arterial pressure is likely multifactorial, involving the effects of general anesthetic agents and opioids, as well as β₂-mediated vasodilation in skeletal muscle (25-30).
Thermoregulation
Patients undergoing large-volume liposuction are at an increased risk of intraoperative and early postoperative hypothermia. This risk arises from several procedural and environmental factors, including exposure of large body surface areas, infusion of large volumes of relatively cold wetting solutions, prolonged operative times, general anesthesia, heat loss during mechanical ventilation, low ambient operating room temperature, and administration of intravenous fluids (38-40).
Hypothermia can have serious physiological consequences, such as cardiac dysrhythmias, coagulopathies, oliguria, and electrolyte imbalances. These complications may be exacerbated by even mild reductions in core body temperature, and both hemodynamic and thermoregulatory disturbances can persist for more than 24 hours after the start of surgery (25).
Postoperative Care
In the postoperative care, it is important to monitor the patients, especially those undergoing large-volume liposuction. Postoperative monitoring should continue beyond the immediate recovery period to observe f delayed hemodynamic changes, fluid shifts, and complications, such as pulmonary edema or fat embolism. The analgesia provided by the tumescent local anesthetic often results in minimal postoperative pain requirements. Adding epinephrine to lidocaine prolongs analgesia for several hours. When appropriate, non-steroidal anti-inflammatory drugs (NSAIDs) can be prescribed postoperatively for additional pain control. Early movement after surgery should be encouraged as soon as possible. Lower extremity muscle-contracting exercises, early mobilization, adequate hydration, and low-molecular-weight heparin reduce the risk of venous stasis and deep vein thrombosis (DVT) (38-40).
Complications
Although liposuction is frequently performed as a day-case procedure, it carries potentially serious complications, particularly with large volumes of aspirate. The overall complication rate for liposuction is approximately 5%, with most being minor; however, major systemic complications and deaths have been reported (40-42). Serious postoperative complications include: deep vein thrombosis (DVT), pulmonary embolism (PE), pulmonary edema and fluid overload, local anesthetic toxicity, infection and sepsis, including rare cases of necrotizing fasciitis or visceral perforation. The incidence of mortality associated with liposuction varies across studies but is estimated to be rare yet significant, especially when large volumes are aspirated, procedures are prolonged, or surgery is combined with other major operations. (41)
The most frequent late complications are unfavorable aesthetic outcomes following liposuction or fat grafting, often requiring subsequent surgical management (42).
Discussion
Tumescent local anesthesia (TLA) with adjunctive remifentanil and dexmedetomidine offers advantages over general anesthesia and sedation alone for many liposuction procedures: it provides prolonged local analgesia and reduced blood loss (epinephrine vasoconstriction), lowers postoperative pain scores, and often allows for ambulatory treatment with faster recovery and lower costs. The remifentanil–dexmedetomidine combination yields rapid, easily titratable analgesia and cooperative sedation that preserves patient responsiveness—facilitating intraoperative communication and safe repositioning—while reducing total opioid requirements and postoperative nausea (12,14,17). Compared with regional or MAC alone, this regimen gives superior control during painful moments (infiltration/aspiration) and greater hemodynamic stability than high-dose opioids, but both agents carry risks: remifentanil can cause respiratory depression and chest-wall rigidity (especially with large boluses) and dexmedetomidine produces dose-dependent bradycardia and hypotension; these effects may be additive when used in combination. The main persistent safety concern with high-volume TLA remains LAST; therefore, strict lidocaine dose calculation, tailored concentrations, slow infiltration, continuous capnography and hemodynamic monitoring, and readiness with airway equipment, lipid emulsion, reversal agents, and vasopressors are mandatory. Evidence favors TLA with or without analgosedation for many cutaneous/subcutaneous procedures; however, heterogeneity in dosing and limited RCT data mean that the choice should be individualized based on patient comorbidities, procedural extent, and available facility resources (19,25,27,29).
Lidocaine systemic toxicity remains a critical risk when large tumescent volumes are used; therefore, precise calculation of total lidocaine dose is mandatory (commonly cited upper limits ~35 mg/kg, though local protocols vary). The existing literature is limited by heterogeneity in dosing regimens, small sample sizes, retrospective designs, and few RCTs specifically evaluating the remifentanil and dexmedetomidine combination in tumescent liposuction (20,21).
The use of lidocaine concentrations and volumes has to be tailored to the patient’s weight and comorbidities. Remifentanil should be administered in small boluses or as a low-rate infusion (avoid large rapid boluses). The same applies to the use of dexmedetomidine It is mandatory to have reversal agents and resuscitation equipment immediately available (naloxone, airway devices, vasopressors, atropine)(13,19,29).
Conclusion
Liposuction is a widely performed procedure for the removal of excess adipose tissue and is associated with significant hemodynamic and physiological perturbations, particularly in large-volume cases. Anesthetic management for liposuction demands a comprehensive understanding of these physiological changes and a proactive approach to anticipate and mitigate potential complications. Meticulous intraoperative monitoring and strict adherence to established fluid therapy and anesthesia guidelines are essential to optimize patient safety and surgical outcomes.
The combination of dexmedetomidine and remifentanil is an effective and safe regimen for sedation and analgesia in liposuction anesthesia. Evidence indicates that this combination provides stable hemodynamics, facilitates adequate analgesia and sedation, and maintains respiratory function with minimal compromise. Compared with alternative sedative-analgesic strategies, adjunctive use of dexmedetomidine with remifentanil has been shown to enhance patient and surgical team satisfaction, reduce intraoperative opioid requirements, and contribute to improved postoperative outcomes, including better sleep and reduced anxiety levels. Furthermore, this combination may be associated with fewer episodes of respiratory depression, sinus bradycardia, and patient movement during the procedure, contributing to a smoother intraoperative course and overall perioperative experience.
References:
- International Society of Aesthetic Plastic Surgery. ISAPS global survey 2023: full report and press releases. 2024.
- Cleveland Clinic. Liposculpture: what it is, recovery, results & complications. Cleveland Clinic; 2022..
- Facque AR, Ambulatory anesthesia in plastic surgery: review of outpatient procedures including liposuction and anesthesia considerations. Ambulatory Anesthesia. 2015
- Sood J, Jayaraman L, Sethi N. Liposuction: Anaesthesia challenges. Indian J Anaesth. 2011;55(3):220–227
- Ahern RW. History of liposuction and early fat-removal surgery. [PDF on file] — Charles Dujarier’s early 1920s attempt led to complications and delay in adoption;
- Illouz Y-G. Development of safer liposuction methods. Ann Chir Plast Esthet. 1984 — Yves-Gérard Illouz introduced the “wet method” with blunt cannulas to reduce bleeding and improve safety.
- Chittoria RK, Singh O, History of liposuction for body contouring. CosmoDerma. 2022 — Illouz and Fournier refined suction techniques with fluid infiltration, laying the groundwork for modern wet methods and improving safety.
- Yves-Gérard Illouz. Wikipedia — Illouz developed the “wet” method with blunt cannulas and saline infusion to reduce bleeding and facilitate fat aspiration.
- Jeffrey A. Klein. The tumescent technique for liposuction surgery. Amer J Cosm Surg vol 4, issue 4, 1987
- History of liposuction for body contouring. ResearchGate/CosmoDerma 10 -16
- Chittoria RK, Singh O. Indications and techniques of liposuction: evolution to modern body contouring. CosmoDerma. 2022.
- Hoyos AE, Millard JA. VASER-assisted high-definition liposculpture. Aesthet Surg J. 2007;27(6):594–604.
- Venkataram J. Tumescent Liposuction: A Review. J Cutan Aesthet Surg. 2008;1(2):49-56
- Mysore V. Tumescent liposuction: Standard guidelines of care. Indian J Dermatol Venereol Leprol. 2008;
- Uttamani RR, et al. Tumescent local anesthesia for dermatosurgical procedures. J Cutan Aesthet Surg. 2020;;
- Samdal F. Blood loss during liposuction using the tumescent technique. Dermatol Surg. 1994;
- Conroy PH. Tumescent anaesthesia. Br J Plast Surg. 2013;
- Klein JA. The tumescent technique for liposuction surgery. Plast Reconstr Surg. 1995;95(3):581–588
- Wang G, et al. Fluid management in extensive liposuction. Medicine (Baltimore). 2018;97(41):e12753
- Uttamani RR, et al. Tumescent local anesthesia for liposuction and dermatosurgical procedures. J Cutan Aesthet Surg. 2020;
- Liposuction techniques: tumescent formula (Klein) [Internet]. Updated 2023 [cited 2026 Feb 14]. Available from: https://emedicine.medscape.com/
- Ostad A, Kageyama N, Moy RL. Tumescent anesthesia with a lidocaine dose of 55 mg/kg is safe for liposuction. Dermatol Surg. 1996;22(11):921–927.
- Mysore V. Tumescent liposuction: Standard guidelines of care. Indian J Dermatol Venereol Leprol. 2008.
- Venkataram J. Tumescent liposuction: a review. J Cutan Aesthet Surg. 2008;1(2):49–57.
- Mysore V. Tumescent liposuction: standard guidelines of care. Indian J Dermatol Venereol Leprol.2008;74(1):S12–S16
- Lalinde E, Sanz J, Ballesteros A, et al. Effect of L-ornithine 8-vasopressin on blood loss during liposuction. Ann Plast Surg. 1995.
- Parham SM, Pasieka HB. Effect of pH modification by bicarbonate on pain after local anesthetic injection. Anesth Analg. 1996;
- Wallace T, et al. Defining the optimum tumescent anesthesia solution. J Vasc Interv Dermatol. 2017
- Sood J, Jayaraman L, Sethi N. Anti-inflammatory additives in tumescent solutions: effects of steroids on tissue response. Indian J Anaesth. 2011;55(3):220-227.
- Sood J, Jayaraman L, Sethi N. Liposuction: Anaesthesia challenges. Indian J Anaesth. 2011;55(3):220-227.
- Winocour J, Layliev N. Liposuction. In: Editor(s). Book title. Edition. Place of publication: Publisher;2021.
- Guidelines for liposuction surgery. Place of publication: ACCSM; 2023.
- Wang Y, et al. Comparison of dexmedetomidine–remifentanil vs dexmedetomidine– sufentanil in liposuction sedation. BMC Anesthesiol. 2022;22:28
- Chen H, et al. Subanesthetic esketamine improves sedative and analgesic effects of dexmedetomidine–remifentanil for liposuction anesthesia. Drug Des Devel Ther. 2024;18:36453658.
- Liposuction and anaesthesia guidelines. South Afr J Anaesth Analg. 2022;28(5) — capnography with sedation and invasive monitoring considerations in high-risk patients.
- Kenkel JM, et al. Hemodynamic Physiology and Thermoregulation in Liposuction. Aesthet Surg J. 2004;24(4):
- Brazilian Society of Plastic Surgery. Practical criteria for a safer liposuction: a multidisciplinary approach — contraindications, comorbidity optimisation, and medication considerations prior to liposuction.
- Cárdenas-Camarena L, et al. Strategies for reducing fatal complications in liposuction. Plast Reconstr Surg Glob Open. 2017;5(10): e1535
- Kao YM, et al. Pulmonary fat embolism following liposuction and fat grafting: a review of published cases. Healthcare (Basel). 2023;11(10):1391
- Dixit VV, Unfavourable outcomes of liposuction and their management. J Cutan Aesthet Surg. 2013;6(4):191-199.